
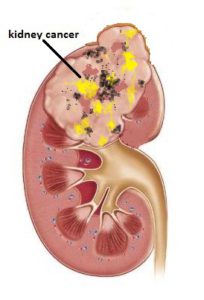
Kidney Cancer
5 Key points:
- The typical presentation of advanced kidney cancer is bloody urine, weight loss and loin ache
- The diagnostic test is CT scan and there is no need to biopsy the tumour to prove cancer
- Early small cancers are increasingly being detected from ultrasound screening
- Total nephrectomy is the standard surgery but partial nephrectomy is feasible if the tumour is small, e.g. less than 4 cm and gives the same cure rate and preserves as much of the kidney to avoid kidney failure in later years
- Laparoscopic partial nephrectomy is a technically more difficult surgery to perform but feasible with the da Vinci robot
Kidney cancer is now the 9th commonest cancer in men here in Singapore. Several types of cancer can develop in the kidney. The most common is renal cell cancer (RCC) which develops from the tubules of the cortex. The most common risk factor is smoking, but genetic factors account for cases that occur in people as young as 30 years. People who have an inherited disorder called Von Hippel Lindau disease are at greater risk of developing kidney cancer. In childhood, a different type of kidney cancer is seen and is called a Wilms’ tumour. This article deals with RCC in adults only.
Symptoms
In the early stages, kidney cancer produces no symptoms. With increasing use of ultrasound during health screening, we are now discovering smaller tumours and at an earlier stage. As the cancer grows in size, the following symptoms occur:
a) Blood in the urine (haematuria) – painless
b) Pain in the loin which is persistent
c) Consitutional symptoms like weight loss, poor appetite. fever and lethargy
Stages
Stage 1 cancer is seen with tumours < 7 cm. As the cancer grows, it can cause bloody urine. By then, it is usually more than 7 cm (Stage 2). In Stage 3, it has grown beyond the kidney to invade its surrounding fat and extend into the major vein. Subsequently, it spreads to the lymph nodes. Distant spread to the lungs and bones finally occurs (Stage 4) [Fig 1].
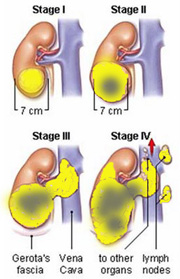
Fig 1. Stages of kidney cancer
Diagnosis
Urine test may detect presence of red blood cells. Ultrasound can also detect tumours when they reach 2 cm size [Fig 2].
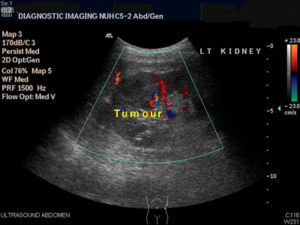
Fig 2. Ultrasound of the kidney can detect incidental and early cancers when they reach 2 cm size
Following ultrasound, the next test required is a CT scan. The CT scan can confirm if the mass is cancerous, as well as show any spread into the renal vein, lymph nodes and adjacent organs [Fig 3]. The CT scan appearance is good enough and there is no need to do a biopsy. If the tumour has invaded into the renal vein or main abdominal vein (IVC), an MRI exam needed. A bone scan is done when bone pain is felt. Finally, a Chest Xray is done to look for any spread to the lungs.
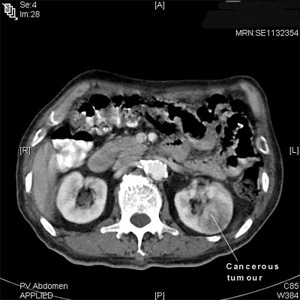
Fig 3. CT scan will confirm if the kidney mass is cancerous
Biopsy is not indicated as most solid masses in the kidney are cancerous in nature. There is also a theoretical risk of seeding the cancer cells along the needle track.
Management
a. Early stage (T1,T2)
The primary management is surgery. A high cure rate is only possible when the cancer is of Stage 1 and 2. For large tumours e.g. > 4 cm, surgery involves removing the whole kidney, adrenal gland and surrounding fat (radical nephrectomy) [Fig 4].
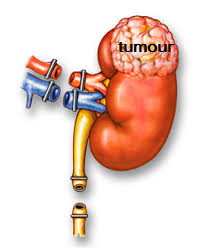
Fig 4. Radical nephrectomy is the removal of the entire kidney including its surrounding fat to ensure complete clearance of the cancer
If the tumour is small (< 4 cm), partial nephrectomy is possible [Fig 5]. This has the advantage of preserving as much remaining kidney as possible; important for those with one kidney or with pre-existing chronic kidney disease (CKD). It will also delay the risk of CKD in the later years – important for those who suffer from hypertension, diabetes and hyperlipidaemia. The cure rate for partial nephrectomy is the same as for radical nephrectomy provided the surgical margins are clear. Laparoscopic and robotic methods are now possible and achieves the same outcomes but with keyhole incisions.
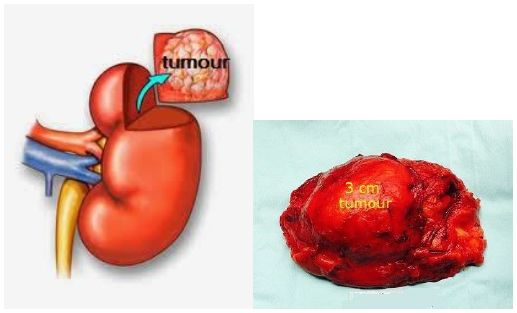
Fig 5. In partial nephrectomy, only the part of the kidney containing the cancer is removed. This is feasible if the tumour is small (< 4 cm)
Interruption of the blood supply to the kidney (arterial embolisation) is sometimes considered before an operation to shrink large and bleeding tumours prior to surgery. This procedure is carried out by the interventional radiologist. Radiotherapy is ineffective for primary kidney cancer and is used more often to treat recurrence after nephrectomy or if there is painful spread to the bones. Radiofrequency ablation is also available but best reserved for elderly patients with small tumours as the effectiveness is unpredictable.
b. Advanced stage (T3, T4)
Patients who have locally advanced cancer (stage T3), nephrectomy is still advised with the aim of removing the source of the cancer. Post- surgery, they will need to take oral chemotherapy drugs, called tyrosine kinase inhibitors (TKI) to control the remaining cancer cells from spreading. However, they are very expensive and need to be taken indefinitely. Disseminated kidney cancer carries a poor prognosis. New immunotherapy drugs have limited response and is expensive with many side effects.
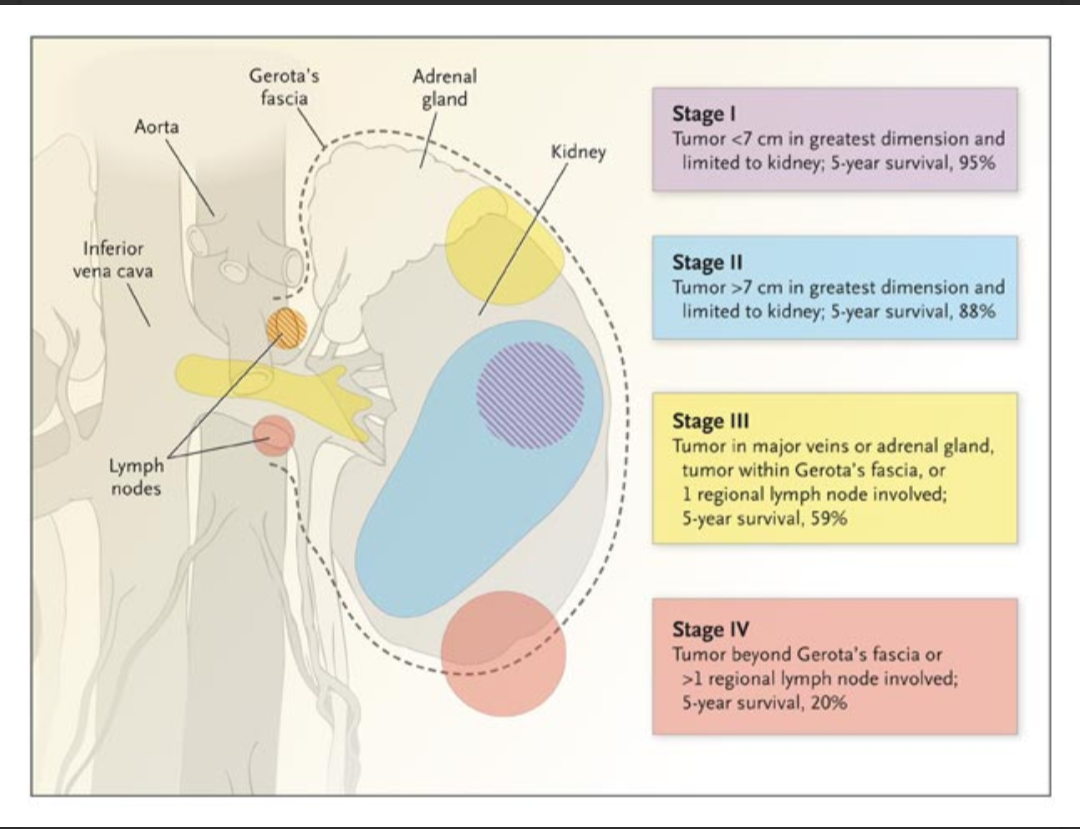
Stage & Prognosis of Kidney Cancer
Summary
It is important to detect kidney cancer at Stage 1 because this gives the best prognosis. It would be even better if the tumour is picked up while it is small ( < 4 cm in size ) because it would still be possible to do a partial nephrectomy and spare as much of the kidney to avoid kidney failure in the future years. Robotic-assisted laparoscopy is the preferred choice to keep the ischaemia time < 30 mins with a water-tight kidney repair.